However, because our patient had a history of late posttraumatic seizure, we changed his medication from phenytoin to carbamazepine, a safer alternative, rather than stop his anti-seizure treatment. 6 Seizure prophylaxis is not indicated in all cases of posttraumatic seizure. It is diagnosed clinically when a patient has gingival enlargement, is taking a medication from one of the causative classes, and has no intraoral or general physical examination features that suggest an inflammatory, hereditary, or systemic condition.ĭiscontinuing the offending drug coupled with meticulous oral hygiene may lead to resolution, but surgical intervention to the gingiva is usually required. Secondary inflammation of these lesions leads to gum bleeding and discomfort with chewing or toothbrushing. 6ĭrug-induced gingival overgrowth usually presents as enlargement of gingival tissue that encroaches on the tooth crowns. 5 It has a direct action on high-activity gingival fibroblasts, and the related severity of gingi-val enlargement is dose-dependent. Gingival hyperplasia is a condition when the gum tissue becomes enlarged and gingival cells increase in number. 4 Phenytoin is the most common culprit, and gingival enlargement is reported in up to 50% of patients who take the drug. Gingival Hyperplasia: Differential Diagnosis Associations: Bleeding gums especially with eating, flossing or brushing teeth Pathophysiology: Inflammation. In addition to gingival overgrowth, there was hypertrichosis over the upper and lower extremities.ĭrug-induced gingival overgrowth is a notable side effect of anticonvulsant drugs (phenytoin, vigabatrin, ethosuximide, topiramate, lamotrigine, valproate, phenobarbital), immunosuppressants (cyclosporine, tacrolimus, sirolimus), and calcium channel blockers (nifedipine, felodipine, verapamil, diltiazem). 
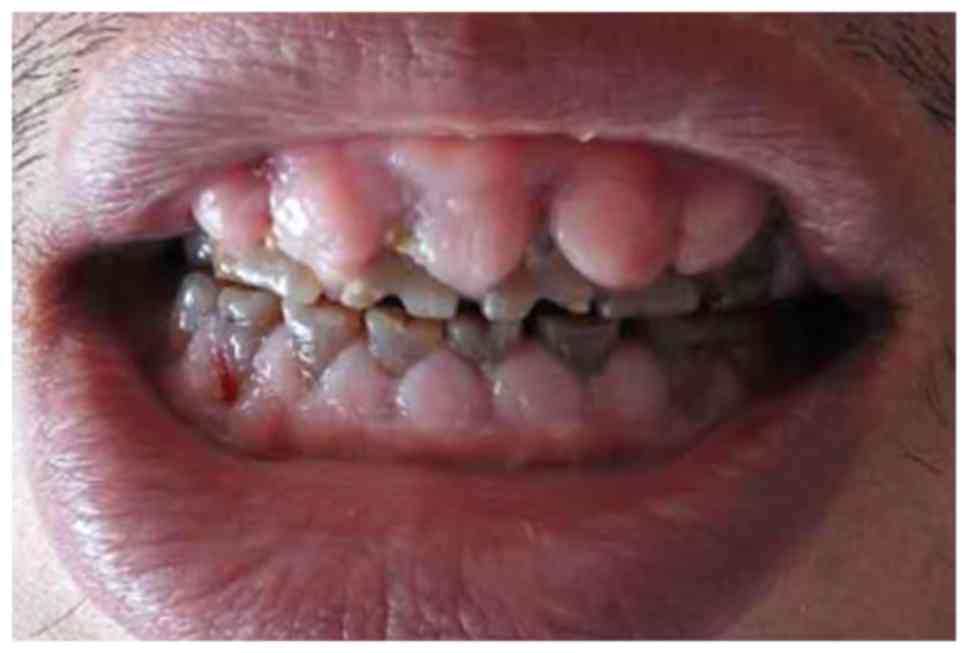
The gingival lesions did not bleed on probing but were tender and suppurative at some places. The gingival swelling covered more than one-third of the tooth crown in the upper row and more than two-thirds in the lower row ( Figure 1). Intraoral examination revealed generalized puffy, lobulated, swollen gums in the upper and lower jaws. No other abnormalities were noted relative to gait, reflexes, or autonomic function, and he had no nystagmus or confusion. Nerve conduction studies showed increased latency and decreased conduction velocity in major nerves of the lower limbs. On examination, a Medical Research Council grade of 4/5 was noted bilaterally in his lower limbs. The patient had no past history of significant neuro logic abnormalities. Alpdogan Kantarci and Hatice Hasturk.A 27-year-old man presented to our neurosurgery clinic with a 3-month history of lower-extremity weakness and slurred speech.Īfter a traffic accident 1 year earlier, he had undergone right decompressive hemicraniectomy to evacuate an acute subdural hematoma, and after an episode of posttraumatic seizure associated with the hemicraniectomy, he was prescribed phenytoin for seizure prophylaxis and has been taking it ever since. Alan Lee, a 2008 graduate of the MSD/CAGS program, with help from Associate Professors of Periodontology & Oral Biology Drs. Siddika Selva Sume, a DSc candidate in Oral Biology and Dr. Trackman hopes to interfere with EMT in mice to determine if overgrowth decreases. “Taken together, the data support our hypothesis that EMT contributes to the pathology of gingival overgrowth,” Dr. He also looked at the ability of TGF-β1, a factor that drives gingival overgrowth, to stimulate EMT in primary human gingival epithelial cells in vitro. Trackman looked for loss of epithelial cell markers and gain of fibroblastic markers in the epithelium, and gain of markers of fibrosis in the connective tissue stroma in human tissue samples in vivo. “EMT was never considered to contribute to gingival overgrowth before, although features of the histopathology were a strong clue for this biological process occurring in all forms of human gingival overgrowth.”ĭr. “EMT is a normal part of embryonic development, but in adults occurs only in disease, specifically cancer and fibrosis,” Dr. Philip Trackman and colleagues show a cellular process called epithelial to mesenchymal transition (EMT) could contribute to gingival overgrowth. Goldman School of Dental Medicine (GSDM) Professor of Periodontology and Oral Biology Dr. In a new study, Boston University Henry M. While it happens for different reasons, drug-induced gingival overgrowth is a well-known side effect of medications including the anti-seizure drug phenytoin, the immunosuppressant cyclosporin A, and calcium channel blockers (to treat high blood pressure) such as nifedipine. When gum tissue grows over the teeth, it’s called gingival overgrowth, and it puts people at risk for gum disease and oral infections, interferes with chewing, and is painful. Study Shows EMT Could Contribute to Harmful Gum Overgrowth
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
